By Kai Kupferschmidt

A 3-year-old boy is treated for cholera in Iquitos, Peru, in 1991, in an epidemic that affected most of Latin America. Credit: ALEJANDRO BALANGUER/AP IMAGES
In perhaps the most famous example of shoe-leather epidemiology, U.K. physician John Snow mapped cholera cases in London in 1854 to pinpoint a water pump on Broad Street as the likely source of a deadly outbreak. Removing the pump handle helped stop its spread. Now, scientists have done similar detective work on a global scale, using 21st-century techniques. By sequencing and comparing hundreds of bacterial genomes, they have shown that all of the explosive epidemics of cholera in Africa and the Americas in the past half-century arose after the arrival of new strains that had evolved in Asia.
The work, published in two Science papers this week, could put to rest an old debate about the role of environmental factors in cholera’s global burden. It could also have a big impact on the battle against the disease, because it allows public health officials to concentrate their efforts on the imported strains that are likely to be the most dangerous. And it suggests there is no local reservoir for major outbreaks in Africa or the Americas, which means “elimination of cholera in these places is completely achievable,” says Dominique Legros, a cholera expert at the World Health Organization (WHO) in Geneva, Switzerland. “This is music to my ears.”
Cholera is caused by the bacterium Vibrio cholerae, which spreads through water contaminated with feces. Over the centuries, dangerous strains of the bacterium appear to have spread from Asia to the rest of the world in several waves. The latest, called the seventh pandemic, began in 1961 and is ongoing, causing an estimated 3 million cases each year.
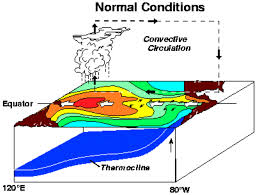
In the 1970s, however, Rita Colwell of the University of Maryland in College Park suggested that outbreaks could originate in the local environment. She showed that V. cholerae lives in many rivers and coastal waters, including the Chesapeake Bay, a large estuary on the east coast of the United States. The bacteria attach themselves to plankton; Colwell argued that when climatic events such as El Niño trigger plankton blooms, cholera can erupt in areas with bad sanitation. Climate change could make such outbreaks more frequent, she warned.
Since then experts have debated how many big cholera outbreaks are caused by such local events rather than brought in by travelers. “The community has been completely fractured by this,” says Nicholas Thomson, a researcher at the Wellcome Trust Sanger Institute in Hinxton, U.K. Some have proposed combinations of the two scenarios; Africa, for instance, has had about a dozen big outbreaks in the past 50 years, and one theory holds that an Asian strain of V. cholerae was introduced once and then established itself in the environment, says Marco Salemi, a molecular epidemiologist at the University of Florida’s Emerging Pathogens Institute in Gainesville. Imported microbes could also swap genes with local populations to create new strains. “If you spent time going though all the literature, you’d simply be confused,” Thomson says.
Cholera’s travels
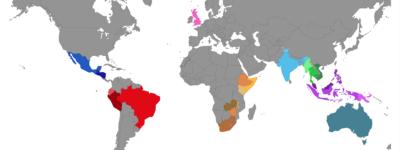
The two major cholera epidemics that occurred in the Americas in the past 50 years were both caused by imported strains. So were 11 African epidemics.

To solve the problem, Thomson and an international team of researchers spent years assembling a collection of 714 bacterial isolates spanning half a century in Asia, Africa, and the Americas. They sequenced all of them and compared the genomes, along with hundreds more that had been published before.
The picture that emerged is strikingly clear. The Americas have seen two major cholera outbreaks in the past half-century: one that began in Peru and raced through almost all of Latin America between 1991 and 1993, and another in Haiti that started in 2010 and is ongoing. The analysis confirms previous strong evidence that the Haiti outbreak was inadvertently introduced by United Nations peacekeepers from Nepal, and it shows that the ’90s outbreak was also caused by Asian strains, both introduced in 1991. One arrived in Peru by way of Africa, and the other landed in Mexico, having traveled from southern Asia, possibly via Eastern Europe. In Africa, the researchers could pinpoint 11 separate introductions of cholera from Asia that went on to cause massive outbreaks. Local strains did sometimes cause disease in both Africa and Latin America, but none led to an explosive epidemic.
The two papers “make the environmental hypothesis untenable, at least in the form that has been most aggressively promoted,” says microbiologist John Mekalanos of Harvard Medical School in Boston. “I certainly hope this puts this theory to rest.” Salemi says he was surprised by the results, particularly in Africa. “I would have expected to see more locally generated outbreaks,” he says, but “the analysis they do and the data they show are very clear.”
Colwell—whose cholera research and advocacy for clean water have earned her many plaudits, including the National Medal of Science—told Science she did not want to publicly discuss the new research. Colwell says she has been “treated terribly” by her opponents in the long-running debate: “I’ve had 30 years of being dumped on and I don’t want to be dumped on anymore.”
Last month, WHO unveiled a plan to cut cholera deaths by 90% by 2030 by improving access to safe drinking water and by deploying an oral cholera vaccine, a stockpile of which was created in 2013. The new research will help those efforts, Legros says. When a new cholera case appears, researchers can now sequence the bacterium to determine whether it belongs to the pandemic lineage from Asia. That could help pinpoint truly dangerous outbreaks that most warrant use of the limited vaccine stocks, Thomson says: “The simple fact that you can now distinguish this form from all other cholera means that we have a chance to do something about it.”
But the research also highlights the importance of eliminating natural reservoirs of pandemic V. cholerae in Asia. “If we want to control cholera at the global level, we must control it in that part of the world,” Legros says. Something in the region allows new strains to evolve and spread across the world, and scientists aren’t sure what it is. “The ecology there is almost certainly different from elsewhere,” Thomson says. It’s as if scientists have identified the pump, but not yet a handle they can pull
Categories: Health